|
||
|
||
|
Effective December 27, 2020, federal law prohibits health plans and issuers from entering into a contract with a health care provider, TPA, or other service providers that contains a gag clause.
Group health plans and health insurance issuers offering group or individual health insurance coverage must annually submit a Gag Clause Prohibition Compliance Attestation (GCPCA) to the Departments of Labor, Health & Human Services, and the Treasury.
The gag clause attestation is due by December 31, 2025 and will cover the period since the preceding attestation.
If you would like to learn more about the gag clause, please visit the following link: Gag Clause Prohibition Compliance Attestation CMS
What do you need to do?
Either the employer or the carrier/TPA needs to attest to the gag clause.
See the table below (click to download) for who is responsible for completing the attestation:
|
||
|
|
||
**If you have any level funded plans with BCBSMN, please let us know by November 26th if you would like help filing on behalf of your employer.
***UnitedHealthcare provides a confirmation of compliance for self-funded groups to attest.
If the employer needs to complete attestation:
- Get confirmation of compliance from carrier/TPA
- Follow the attached link to the attestation: Enter Webform Now for a GCPCA
- The following link contains step-by-step instructions to help guide you through the process of submitting your attestation: User Manual for submitting the GCPCA
Please Note: If a plan carves out pharmacy benefit management or mental health, the plan is responsible for the gag attestation on the carveout entity arrangement.
If your group has any of the following plans, they do not need to complete the attestation:
- Account-based plans, such as health reimbursement arrangements (HRAs), including individual coverage HRAs.
- Issuers and group health plans that offer only excepted benefits coverage, including, but not limited to:
- Hospital indemnity or other fixed indemnity insurance
- Disease-specific insurance
- Dental, vision, and long-term care
- Accident-only, disability, and workers’ compensation
- Issuers that offer only short-term, limited-duration insurance
- Medicare and Medicaid plans
- State children’s health insurance program plans
- Basic Health Program plans
Questions? Please contact our team at groupadmin@ociservices.com or give us a call us at (402) 330-8700.
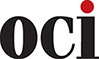




![[Action Required] Medica’s New Broker Portal Launch](https://www.ociservices.com/wp-content/uploads/Updated-Date-Medica-New-Broker-Portal-Launch-500x383.jpg)
![[Deadline Approaching] RxDC Reporting Requirements](https://www.ociservices.com/wp-content/uploads/RxDC-Reporting-500x383.png)